The science once confined to weight loss is now rewriting the future of medicine.
Table of Contents
Just a few years ago, GLP-1 drugs were seen as powerful—but narrow—tools for diabetes and obesity.
Now?
They’re reshaping cardiology, neurology, hepatology, nephrology, psychiatry, and preventive medicine.
As of 2026, GLP-1 drugs are no longer just metabolic medications. They are becoming a platform technology for chronic disease treatment.
And the transformation is only beginning.
The GLP-1 Revolution No One Saw Coming
GLP-1 drugs (glucagon-like peptide-1 receptor agonists) mimic a natural hormone involved in:
- Insulin regulation
- Appetite control
- Gastric emptying
- Glucose metabolism
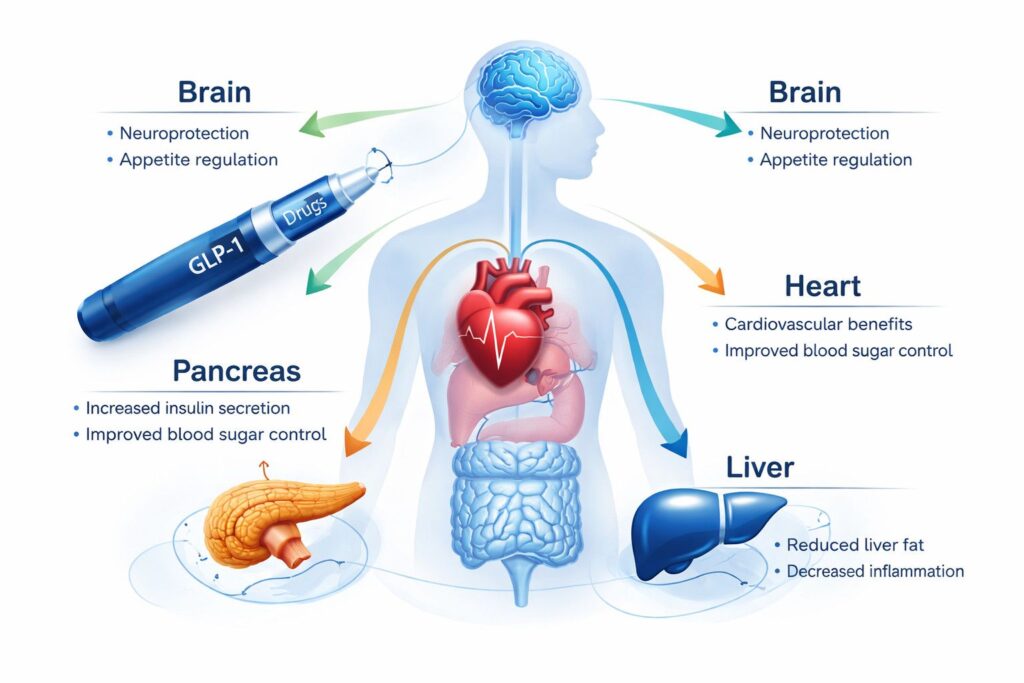
But researchers quickly discovered something bigger: GLP-1 receptors exist throughout the body — including the heart, brain, kidneys, and liver.
That discovery changed everything.
Major clinical trials over the past three years have expanded their indication far beyond weight loss:
- SELECT trial (cardiovascular outcomes)
- FLOW trial (kidney protection)
- Ongoing trials in Alzheimer’s and addiction medicine
The result? GLP-1 drugs in 2026 are being positioned as multi-system disease modifiers.
Why 2026 Is the Tipping Point for GLP-1 Drugs
Three forces collided:
- Massive outcome trials proving cardiovascular benefit
- Regulatory expansion into new indications
- Explosive biotech investment into next-generation GLP-1 drugs
In 2023, the SELECT cardiovascular outcomes trial demonstrated that semaglutide reduced major adverse cardiovascular events in overweight patients without diabetes. This was published in the New England Journal of Medicine:
https://www.nejm.org/doi/full/10.1056/NEJMoa2307563
That study changed prescribing behavior globally.
By 2026, cardiologists are discussing GLP-1 drugs alongside statins.
That’s not incremental change.
That’s a paradigm shift.
Shocking Shift #1: GLP-1 Drugs Are Becoming Heart-Protective Powerhouses
For decades, obesity drugs were judged by one metric: weight reduction.
Now they’re being evaluated by survival.
The SELECT trial showed a significant reduction in:
- Heart attack
- Stroke
- Cardiovascular death
This elevated GLP-1 drugs from cosmetic perception to life-saving therapy.
Why it matters:
- Cardiovascular disease remains the leading global killer.
- Even modest risk reductions scale dramatically across populations.
GLP-1 drugs in 2026 are increasingly prescribed for cardiovascular risk reduction—even in non-diabetic patients.
This changes:
- Insurance coverage debates
- Prescribing authority
- Public health guidelines
Cardiology may never look the same.
Shocking Shift #2: The Brain Health Breakthrough That Could Change Alzheimer’s Research
Here’s where things get disruptive.
GLP-1 receptors are present in the brain.
Emerging research suggests they may:
- Reduce neuroinflammation
- Improve insulin signaling in neurons
- Protect against cognitive decline
Early-phase trials are investigating semaglutide and similar agents in Alzheimer’s disease.
While definitive outcomes are pending, preliminary data suggests possible cognitive stabilization in high-risk groups.
If confirmed, GLP-1 drugs beyond weight loss could redefine neurodegenerative disease management.
Imagine a metabolic drug influencing dementia progression.
That’s not evolution.
That’s medical disruption.
Shocking Shift #3: Fatty Liver Disease May Finally Have a Real Treatment
Nonalcoholic steatohepatitis (NASH) — now called MASH — affects millions globally.
Until recently, treatment options were limited.
GLP-1 drugs have shown promising results in:
- Reducing liver fat
- Improving liver inflammation
- Supporting fibrosis regression
A 2021 study in The New England Journal of Medicine demonstrated histologic improvements in NASH patients treated with semaglutide:
https://www.nejm.org/doi/full/10.1056/NEJMoa2028395
By 2026, GLP-1 drugs are being positioned as frontline metabolic liver therapies.
That could dramatically reduce:
- Cirrhosis progression
- Liver transplant demand
- Long-term healthcare costs
This alone could shift hepatology guidelines worldwide.
Shocking Shift #4: Addiction Medicine Is Entering a New Era
This is one of the most unexpected developments.
Researchers are exploring GLP-1 drugs for:
- Alcohol use disorder
- Nicotine dependence
- Opioid cravings
Why?
GLP-1 pathways interact with dopamine reward systems.
Early animal and small human studies suggest reduced addictive behaviors when GLP-1 drugs are administered.
If large trials confirm this, addiction medicine could gain a metabolic intervention tool—something previously unimaginable.
Addiction has long been treated psychologically and behaviorally.
GLP-1 drugs may introduce a biological lever.
That changes stigma.
That changes strategy.
Shocking Shift #5: Kidney Protection Is Reshaping Chronic Disease Care
Chronic kidney disease (CKD) is a silent epidemic.
In 2024–2025, the FLOW trial demonstrated kidney-protective benefits in patients with diabetes and CKD.
This expanded the conversation from glucose control to organ preservation.
By 2026, nephrologists are incorporating GLP-1 drugs into kidney risk management frameworks.
Combined with SGLT2 inhibitors, this creates a new dual-protection model.
The implication?
GLP-1 drugs beyond weight loss are becoming foundational chronic disease medications.
Shocking Shift #6: GLP-1 Drugs Are Redefining Preventive Medicine
Here’s the real disruption:
GLP-1 drugs in 2026 are entering preventive care conversations.
Instead of waiting for:
- Diabetes
- Heart attack
- Liver failure
Doctors are discussing earlier metabolic intervention.
The logic is simple:
Metabolic dysfunction drives multiple chronic diseases.
Correct it early.
Reduce downstream cost.
This shifts healthcare from reactive to proactive.
And insurers are watching closely.
Shocking Shift #7: The Rise of Next-Gen Dual & Triple Agonists
The first wave was GLP-1 alone.
The second wave?
Multi-agonists.
Drugs that target:
- GLP-1
- GIP
- Glucagon receptors
Tirzepatide (a dual GLP-1/GIP agonist) has already demonstrated superior weight and metabolic outcomes compared to earlier agents.
Biotech pipelines in 2026 are racing toward triple-agonist combinations designed to amplify metabolic effects.
This isn’t just improvement.
It’s iteration at scale.
The metabolic drug class is evolving like smartphones did between 2007 and 2015.
Rapid. Competitive. Transformative.
The Economic Earthquake: Healthcare Systems Will Never Be the Same
GLP-1 drugs are expensive.
That creates tension:
- High upfront drug cost
- Potential long-term savings
If these medications prevent:
- Heart attacks
- Dialysis
- Liver transplants
- Dementia progression
The economic calculus shifts dramatically.
Governments and insurers are running cost-effectiveness models now.
Because if GLP-1 drugs reduce multi-organ disease burden…
They could become the statins of the 2030s.
The Risks, Limits, and Ethical Questions We Can’t Ignore
Not everything is revolutionary upside.
Known concerns include:
- Gastrointestinal side effects
- Pancreatitis risk (rare but monitored)
- Long-term safety beyond 10+ years
- Equity of access
There are also social questions:
- Will preventive GLP-1 use widen healthcare inequality?
- Should these drugs be prescribed broadly?
- What happens if supply shortages persist?
Medical transformation must be matched with ethical oversight.
What Happens Next? The Future of GLP-1 Drugs Beyond 2026
Here’s what experts are watching:
- Alzheimer’s trial outcomes
- Addiction medicine data
- Pediatric metabolic use
- Long-term cardiovascular mortality follow-up
- Oral GLP-1 formulations improving access
GLP-1 drugs in 2026 are not the endpoint.
They’re the inflection point.
The science once confined to weight loss is now rewriting the future of medicine.
And we’re only in chapter one.
External resources (DoFollow)
Robert Cialdini’s work on reciprocity (Influence): https://www.influenceatwork.com/principles-of-persuasion/
LinkedIn help docs on engagement basics and best practices: https://www.linkedin.com/help/linkedin/